Dental Implants
Dental Implants are the most successful and sometimes the only treatment option for replacing Missing teeth. Whether it is replacing one or all missing teeth, Dental Implants can be the best treatment option for all.
About IMPLANTS @ DENTAL CONCEPTS
- Dental Concepts - Dental Spa and Implant Center
- Dental Concepts was established in 1983 to provide advanced treatment in dental care. It is formed of a team of specialists headed by Dr. Dhimant Gala who is highly accomplished and a successful practitioner with over 25 years of experience. His son, Dr. Jigar D Gala is among the first qualified Dental Implantologist in India to have a Masters Degree in Implant Dentistry from the prestigious UCL-Eastman Dental Institute, London. He practises exclusive Cosmetic and Implant Dentistry and lectures in India and Abroad focussing on the latest trends in Implants.
What are Dental Implants?
A dental implant is a "root" device, usually made of titanium, used in dentistry to support restorations that resemble a tooth or group of teeth to replace missing teeth.
Virtually all dental implants placed today are root-form endosseous implants, i.e., they appear similar to an actual tooth root and are placed within the bone (endo- being the Greek prefix for "in" and osseous referring to "bone"). The bone of the jaw accepts and osseointegrates with the titanium post.
Osseo integration refers to the fusion of the implant surface with the surrounding bone. This is what makes the implant resemble the look and feel of a natural tooth. Dental implants will fuse with bone, however they lack the periodontal ligament, so they will feel slightly different than natural teeth during chewing.
Prior to the advent of root-form endosseous implants, most implants were either blade endosseous implants, in that the shape of the metal piece placed within the bone resembled a flat blade, or subperiosteal implants, in which a framework was constructed to lie upon and was attached with screws to the exposed bone of the jaws.
Dental implants can be used to support a number of dental prostheses, including crowns, implant-supported bridges or dentures.
Composition
A typical implant consists of a titanium screw (resembling a tooth root) with a roughened or smooth surface. The majority of dental implants are made out of commercially pure titanium, which is available in 4 grades depending upon the amount of carbon and iron contained. More recently grade 5 titanium has increased in use. Grade 5 titanium, Titanium 6AL-4V, (signifying the Titanium alloy containing 6% Aluminium and 4% Vanadium alloy) is believed to offer similar osseointegration levels as commercially pure titanium. Ti-6Al-4V alloy offers better tensile strength and fracture resistance. Today most implants are still made out of commercially pure titanium (grades 1 to 4) but some implant systems (Endopore and NanoTite) are fabricated out of the Ti-6Al-4V alloy. Implant surfaces may be modified by plasma spraying, anodizing, etching or sandblasting to increase the surface area and the integration potential of the implant.
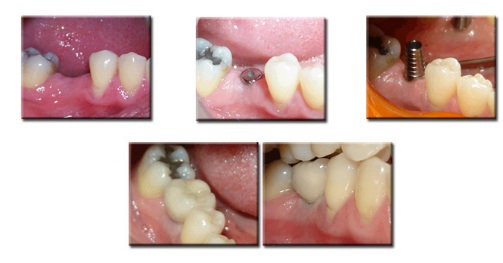
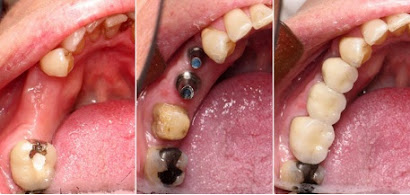
Procedure:
Pre Surgical planning: Prior to commencement of surgery, careful and detailed planning is required to identify vital structures such as the inferior alveolar nerve or the sinus, as well as the shape and dimensions of the bone to properly orient the implants for the most predictable outcome. Two-dimensional radiographs, such as orthopantomographs or periapicals are often taken prior to the surgery. Sometimes, a CT scan will also be obtained. Specialized 3D CAD/CAM computer programs may be used to plan the case.
Surgical incisions: Traditionally, an incision is made over the crest of the site where the implant is to be placed. This is referred to as a 'flap'. Some systems allow for 'flapless' surgery where a piece of mucosa is punched-out from over the implant site. Proponents of 'flapless' surgery believe that it decreases recovery time while its detractors believe it increases complication rates because the edge of bone cannot be visualized.
Surgical procedure: At edentulous (without teeth) jaw sites, a pilot hole is bored into the recipient bone, taking care to avoid the vital structures Drilling into jawbone usually occurs in several separate steps. The pilot hole is expanded by using progressively wider drills, depending on implant width and length. A cooling saline or water spray keeps the temperature of the bone to below 47 degrees. The implant is screwed into place at a precise torque so as not to overload the surrounding bone.
Surgical timing
There are different approaches to place dental implants after tooth extraction. The approaches are:
- Immediate post-extraction implant placement.
- Delayed immediate post-extraction implant placement (2 weeks to 3 months after extraction).
Healing time
The amount of time that practitioners allow the implant to heal before placing a restoration on it varies widely. In general, practitioners allow 2–6 months for healing but If the implant is loaded too soon, it is possible that the implant may move which results in failure.
Restorative Phase
After the healing period, is the time of restoration or placing the Porcelain teeth over the Implants. This Involves a series of Appointments wherein initially the Implant head is exposed and a healing cap is placed over the head for healthy gums to form around it. Then a measurement is taken with special Impression materials which is send to Dental Lab for making the Prosthesis (Porcelain Crown/Bridge or removable Dentures). Finally the healing cap is replaced with a prosthetic Abutment on which the Prosthesis is either screwed or cemented.
Complementary procedures
Sinus lifting is a common surgical intervention. The Surgeon thickens the inadequate part of atrophic maxilla towards the sinus with the help of bone transplantation or bone expletive substance. This results in more volume for a better quality bone site for the implantation.
Bone grafting will be necessary in cases where there is a lack of adequate maxillary or mandibular bone in terms of depth or thickness. Sufficient bone is needed in three dimensions to securely integrate with the root-like implant. A wide range of grafting materials and substances may be used during the process of bone grafting / bone replacement. They include the patient's own bone (autograft), which may be harvested from the hip (iliac crest) or from spare jawbone; processed bone from cadavers (allograft); bovine bone or coral (xenograft); or artificially produced bone-like substances calcium sulfate. Alternatively the bone intended to support the implant can be split and widened with the implant placed between the two halves like a sandwich.
Success rates
Dental implant success is related to operator skill, quality and quantity of the bone available at the site, and the patient's oral hygiene. The consensus is that implants carry a success rate of around 95%.
One of the most important factors that determine implant success is the achievement and maintenance of implant stability. Other contributing factors to the success of dental implant placement, as with most surgical procedures, include the patient's overall general health and compliance with post-surgical care.
Failure
Failure of a dental implant is often related to failure to osseointegrate correctly. A dental implant is considered to be a failure if it is lost, mobile or shows peri-implant (around the implant) bone loss of greater than 1.0 mm in the first year and greater than 0.2mm a year after.
Dental implants are not susceptible to dental caries but they can develop a condition called peri-implantitis. This is an inflammatory condition of the mucosa and/or bone around the implant which may result in bone loss and eventual loss of the implant. The condition is usually, but not always, associated with a chronic infection. Peri-implantitis is more likely to occur in heavy smokers, patients with diabetes, patients with poor oral hygiene and cases where the mucosa around the implant is thin.
Risk of failure is increased in smokers. For this reason implants are frequently placed only after a patient has stopped smoking as the treatment is very expensive. More rarely, an implant may fail because of poor positioning at the time of surgery, or may be overloaded initially causing failure to integrate. If smoking and positioning problems exist prior to implant surgery, clinicians often advise patients that a bridge or partial denture rather than an implant may be a better solution.
In the majority of cases where an implant fails to integrate with the bone and is rejected by the body the cause is unknown. This may occur in around 5% of cases. To this day we still do not know why bone will integrate with titanium dental implants and why it does not reject the material as a 'foreign body'.
Contraindications
There are few absolute contraindications to implant dentistry. However, there are some systemic, behavioral and anatomic considerations that should be assessed.
Particularly for mandibular (lower jaw) implants, in the vicinity of the mental foramen (MF), there must be sufficient alveolar bone above the mandibular canal also called the inferior alveolar canal or IAC (which acts as the conduit for the neurovascular bundle carrying the inferior alveolar nerve or IAN).
Uncontrolled type II diabetes is a significant relative contraindication as healing following any type of surgical procedure is delayed due to poor peripheral blood circulation. Anatomic considerations include the volume and height of bone available. Often an ancillary procedure known as a block graft or sinus augmentation are needed to provide enough bone for successful implant placement.
There is new information about intravenous and oral bisphosphonates which may put patients at a higher risk of developing a delayed healing syndrome called osteonecrosis. Implants are contraindicated for some patients who take intravenous bisphosphonates.
Bruxism (tooth clenching or grinding) is another consideration which may reduce the prognosis for treatment. The forces generated during bruxism are particularly detrimental to implants while bone is healing; micromovements in the implant positioning are associated with increased rates of implant failure.